Muscle Weakness: Berlin Scientists Unravel Defects in Rare Hereditary Disease Myotubular Myopathy
Study by Leibniz Institute für Molecular Pharmacology and Freie Universität Berlin in Cooperation with Institut Génétique Biologie Moléculaire Cellulaire (IGBMC), Strasbourg and European Molecular Biology Laboratory, Heidelberg
№ 016/2016 from Jan 20, 2016
Tiny deviations in the body's cells can sometimes have severe consequences. Researchers from Berlin have discovered why cells from patients suffering from the rare muscular disease myotubular myopathy cannot function properly. Through the paper published in Nature, it has become clear how a dynamic cellular process essential to muscle development and function is regulated by means of minute changes of certain membrane lipids.
If a child is born with myotubular myopathy, the most severe form of centronuclear myopathies (also called XLCNM), it is barely able to breathe independently. The muscles are atrophied, the newborn lies limp in its mother's arms and is too weak to feed. Babies with this rare muscular disease might not survive the first few months of their lives. The group of Volker Haucke from the Leibniz Institute for Molecular Pharmacology (FMP) and Freie Universität (FUB) in Berlin, in collaboration with the laboratories of Jocelyn Laporte from the Institut Génétique Biologie Moléculaire Cellulaire (IGBMC) in Strasbourg and Carsten Schultz at the European Molecular Biology Laboratory (EMBL) in Heidelberg, has been researching what goes wrong in this disease at the molecular level – and has now come across a general organizational principle in cells.
Up to now, it has been known that this hereditary disease involves a defect in the gene MTM1, as a result of which muscle fibers do not function normally. The gene codes for an enzyme that is specialized in cleaving phosphate groups from the heads of certain membrane lipids called phosphoinositide phosphates (PIPs) but how this leads to disease was unknown. PIPs are used by the cell to tag its compartments and to regulate the transport of substances. "The cell is a very dynamic system, which one can imagine as a metropolis in which the people move back and forth," explains Volker Haucke. "Depending on the occasion, the people change their clothes – if you put on a dress coat, to some extent you assume a different identity than if you come along in jeans and sweatshirt, and you won't be let in to the opera in pyjamas. In a similar manner, the compartments and transport vesicles within cells are constantly putting on different PIPs and thus change their identity." Each PIP consists of a fat-soluble tail that is anchored in the membranes of the cell compartments, and a water-soluble head that protrudes from the membrane. The head can be loaded with phosphates at different sites, the phosphate groups are detached by enzymes and attached at other sites. This is a minimal change that takes place in a flash, yet it is unmistakably read by the cell. Thus, for example, if a phosphate group tags a certain position, it is clear that a transport container is supposed to be transported into the interior of the cell; if the phosphate tag is different, it migrates to the outer cell membrane, docks there, and unloads its freight to the outside.
This kind of transport comes to a halt in XLCNM patients, as could be shown by Katharina Ketel from the Haucke group with intricate experiments and high-resolution images from inside the cell. The cause of the disease is a defect in MTM1, an enzyme that removes phosphate groups from the PIPs and only works in co-operation with another enzyme that attaches a phosphate group to another site on the head. This clarifies how dynamic processes in cells are directed and illustrates how studying a rare genetic disease can discover an essential molecular mechanism for our cells to function properly. "In healthy cells, phosphate groups are never randomly removed from PIPs, because a cell compartment would then suddenly be left completely without an identity – that would be equivalent to a loss of memory. The compartment would no longer know where it's from and where it's supposed to go," explains Volker Haucke. “By adding synthetic PIPs with a certain code, we were able to alter the transport of containers, demonstrating that conversion of PIP identity really is the problem in XLCNM patient cells," adds Carsten Schultz.
"In XLCNM patients, some of the transport containers that were originally supposed to convey proteins to the cell surface get stranded inside the cell because a phosphate group cannot be removed from a certain PIP," says Jocelyn Laporte, an expert in XLCNM and contributor to the study. "In muscles, this may mean that proteins necessary for their formation, integrity, and function do not get to the right place in the cell." In their experiments in cell culture, the FMP researchers were able to restart the transport with a certain active substance. This might be a starting point for the development of drugs for treating this severe and currently incurable hereditary disease.
Press Images
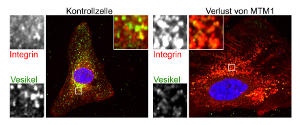
Figure 1: Accumulation of integrin (red), an important component of muscles, in vesicles (green) from cells without MTM1 (right images including magnified view) or from control cells (left images including magnified view). Image Credit: Katharina Ketel, Leibniz Institute for Molecular Pharmacology (FMP), Berlin.
More Information and Interview Requests
Prof. Dr. Volker Haucke, Leibniz Institute for Molecular Pharmacology and Freie Universität Berlin, Tel.: +49 30 947 93 101, Email: haucke@fmp-berlin.de
Link to the Publication:
www.nature.com/nature/journal/vaop/ncurrent/full/nature16516.html