An Underestimated Risk
At a collaborative research center, researchers are working to find answers to previously unresolved questions involving lung inflammations and infections.
Apr 14, 2015
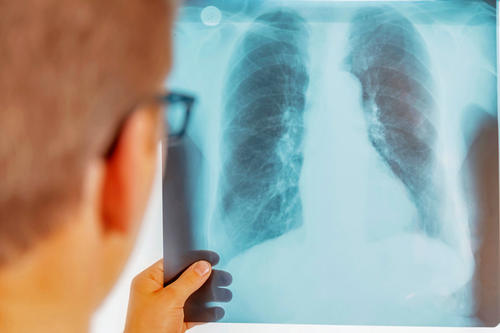
Inflammatory increases in tissue density are often readily apparent in X-ray images of patients with bacterial pneumonia. What exactly happens in the lungs when they are infected with pathogens such as pneumococci has not yet been investigated.
Image Credit: iStockphtoto/Remains
Each year 740,000 people in Germany contract some form of pneumonia outside a hospital. About one-third of them become so sick that they require inpatient treatment. Even with medical attention, twelve percent do not survive the infection.
“That means that the course of the disease in pneumonia is similar in severity to a heart attack or stroke,” says Norbert Suttorp, the director of the Medical Department, Division of Infectiology and Pneumonology at Charité – Universitätsmedizin Berlin, the joint medical school of Freie Universität and Humboldt-Universität zu Berlin. Why is the mortality rate so high despite advances in medicine – and what can be done about it?
Scientists working within the Transregio 84 collaborative research center (CRC) “Innate Immunity of the Lung” funded by the German Research Foundation (DFG) are investigating these issues. The CRC is currently entering the second round of funding. Alongside Charité, the participants are Freie Universität Berlin, the University of Marburg, the University of Giessen, the Robert Koch Institute, the Max Planck Institute (MPI) for Molecular Genetics, in Berlin, and the Max Planck Institute of Colloids and Interfaces, in Potsdam.
Drug Resistance Not Yet a Major Problem in Germany
The researchers are studying things like where exactly the pathogens attack the body, how the human immune system responds to the infection, and how medical practitioners can better assess and predict the course of the disease. “Penicillin resistance in the most important pathogen – pneumococcus bacteria – is not yet a major problem in this country, unlike in the U.S., France, and Italy,” says CRC spokesman Suttorp. That is why the group’s 19 individual projects are also not focusing on new antibiotics, but rather on achieving a more detailed understanding of what actually takes place in the lungs when pneumonia arises.
One thing is clear: The organ has to work very hard. “It has to eliminate the pathogen, but also maintain the gas exchange in the alveoli, tiny air sacs in the lungs, every second at the same time,” Suttorp explains. Thanks to a method known as high-end microscopy, the researchers can watch the alveoli at work, and not just when they are fighting pneumococci. One central technology project is helping them with this through the development of state-of-the-art imaging and histology methods.
To do this, normal tissue margins from lung lobes that have been removed from tumor patients are infected with pathogens that cause pneumonia in the lab and then studied. Refinements of the process aim to use a tiny jet of water to obtain especially thin slices of tissue. The researchers hope this will allow them to clear up pending questions. For a long time, it was unclear, for example, what type of lung cell is affected by the influenza virus. “Under the microscope, we can now see the viruses flitting around in the alveoli and see that it is only the type II epithelial cells that are affected,” Suttorp explains.
MERS Coronavirus Mortality Rate at 50 Percent
The researchers are currently studying a coronavirus from the Middle East Respiratory Syndrome, or MERS, group. The syndrome is an infection of the airways triggered by a new kind of coronavirus. “When we introduce this virus to our tissue samples, truly everything in the alveoli becomes infected,” Suttorp says, adding that this explains why the mortality rate for this particular virus stands at 50 percent. Experiments like these help to explain the mechanisms of infection and develop improved treatments. One entirely new finding is that the lungs are not sterile, but rather are home to microorganisms, much like the intestines. What do the organisms do there? How do they interact? Might they have a protective function?
The researchers in the collaborative research center are also looking into these questions. One special case is the pneumonia that often occurs after a patient has suffered a stroke. “It was previously assumed that this was a kind of aspiration pneumonia, meaning pneumonia caused by problems with swallowing,” Suttorp says. But that turns out not to be the case.
“Stroke patients suffer from a condition called immunoparalysis, especially in the lungs,” he explains. The immune system goes into a shock-like state of paralysis, and just a fraction of the usual number of germs becomes sufficient to cause infection or inflammation. The immune system has to economize in terms of resources, so it deploys its weapons in stages. “If just a single bacterial molecule is traveling in the bloodstream, there isn’t much defense that is required,” Suttorp explains. But if there is something larger there, “it could be a bacterium, and the organism responds by defending itself.”
Charité researchers discovered that the body can even determine whether an invader is dead or alive. If it is alive, the immune system looks for pathogen-associated molecular patterns (PAMPs) within the body, meaning for further signs of life in the pathogen. If these patterns are found, the “red alert” is sounded. This finding will be useful for new vaccines; live vaccines are more effective than those based on inactivated, or killed, pathogens – but they are not as easy to handle, since they have to be refrigerated throughout the process.
“We are trying to produce an inactivated vaccine for pneumococcal bacteria and add PAMPs consisting of snippets of the bacterium’s RNA to it,” Suttorp says. These snippets make the immune system believe that a living pathogen has entered the body, so it brings in the big guns, so to speak. And incidentally, experts in Germany expressly recommend that people ages 60 and over be vaccinated against pneumococcal disease because the risk of infection rises steadily from this age onward.
Which Patients Are Most at Risk of Severe Infection?
Since these bacteria are also responsible for meningitis and middle ear infections, even infants and toddlers are immunized nowadays. According to Suttorp, this also benefits their grandparents: “One study in the United States showed that the prevalence of pneumonia in grandparents decreases if the grandchildren have been vaccinated.”
Doctors are desperately looking for parameters they can use to assess early on which patients will suffer a severe infection. That means genotyping is another major focus for the researchers in this CRC: How do the genes of those who suffer a serious infection with sepsis and therefore require intensive medical care differ from those of patients in whom the infection is less severe? The researchers are also looking for further biological markers in the blood that show the current status of the disease and predict its course.
The very first antibiotic study involving pneumococcal pneumonia, published in 1938 in the medical journal The Lancet, showed the huge role a patient’s own immune system plays in fighting pneumonia. One hundred patients were treated with a sulfonamide drug, while a control group of the same size received a placebo. Seventy of the untreated patients survived – as opposed to 90 of those who had received antibiotics. “We are still working on the last ten percent now,” Suttorp says. “Antibiotics are important. We will always have to use them. But we also need additional treatments that help the body to cope, even if the bacteria have already died off.”
Further Information
- Norbert Suttorp, Director, Medical Clinic for Infectious Medicine and Pneumology, Charité – Universitätsmedizin Berlin, Email: norbert.suttorp@charite.de